Genetic Testing for Pediatric Kidney Disease
Kidney disease is often thought of as an adult-onset condition. While that is the case for many individuals, kidney disease and kidney failure also affect children and adolescents. In fact, almost 10,000 children and adolescents in the United States alone have kidney failure. For that reason, there is a vested interest in understanding the cause and best treatment and management of kidney disease in this young population.
Table of Contents
Clinical causes of chronic kidney disease (CKD)
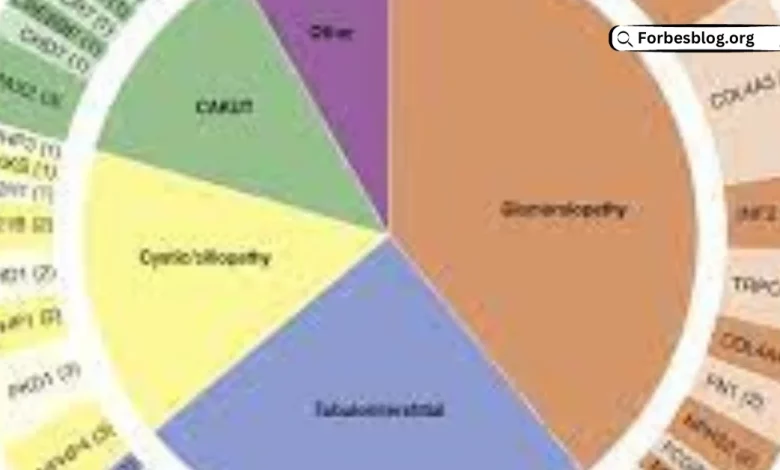
When presenting before 25 years of age, CKD is often (49.1%) related to congenital abnormalities of the kidney or urinary tract (CAKUT). The types of congenital anomalies may include obstructive uropathy, dysplastic kidney, reflux nephropathy, or prune belly syndrome. Approximately 10.4% will have CKD due to steroid resistant nephrotic syndrome, notably focal segmental glomerulosclerosis, congenital nephrotic syndrome, membranous nephropathy, or Denys-Drash syndrome. Chronic glomerulonephritis accounts for 8.1% of cases and may present as systemic lupus erythematosus nephritis, IgA nephritis, or membranoproliferative glomerulonephritis-Type I/II. Other causes of early-onset CKD include renal cystic ciliopathies, hemolytic uremic syndrome, nephrolithiasis/nephrocalcinosis, or other/unknown causes.
Genetic causes of chronic kidney disease (CKD)
While a clinical diagnosis is often made, many cases of early-onset kidney disease also have an underlying genetic cause. Genetic causes or conditions are generally inherited or arise early in development and are not contagious. Vivante and Hildebrant (2016) concluded that about 1 in 5 individuals with early-onset CKD have an identifiable cause. Bekheirnia et al. (2021) identified a genetic cause for 51% of the patients referred to their Renal Genetics Clinic. Genetic conditions previously identified in children/adolescents include, but are not limited, to autosomal dominant polycystic kidney disease, Alport syndrome, renal cysts and diabetes syndrome, Dent disease, Fabry disease, PAX2-related focal segmental glomerulosclerosis, NPHP1-related nephronophthisis, cystinuria, and hereditary angiopathy with nephropathy, aneurysms and muscle cramps.
Genetic testing
There are many approaches to genetic testing for children or adolescents with kidney disease. Genetic testing should be ordered by a provider with knowledge of genetic testing and access to genetic specialists. Given one’s medical and family history, a healthcare provider may wish to order targeted testing which can identify a specific genetic change (variant), variants within one gene, or variants in a small number of genes.
A healthcare provider may also wish to consider a broad panel approach. A broad panel is a genetic test which looks for variants within many genes, often >100. A broad panel approach has become more widely accepted in recent years as one is able to look for a variety of potential diagnoses at one time. This approach can reduce the chance of missing a genetic diagnosis and often is cost effect due to modern next-generation sequencing techniques
Lastly, a healthcare provider may choose the most broad type of genetic testing (whole exome or genome sequencing) which looks for variants within all of our genes (~20,000) with or without non-coding regions. This approach provides the most broad genetic information, but increases the chance of a secondary finding (a genetic result which is unrelated to the patient’s signs or symptoms).
While analyzing specific genes is an important part of genetic testing for most children/adolescents with kidney disease, analysis of copy number variants (cytogenetic analysis or chromosomal microarray) may also be relevant based on an individual’s personal or family history.
Implications of genetic testing
Establishing a genetic diagnosis can impact a patient and their family in many ways. First, having a diagnosis may impact how the patient is being treated now or in the future. For example, individuals with Alport syndrome generally do not respond to immunosuppressive therapy. Oftentimes, this is avoided due to the known side effects of immunosuppressive therapy. Healthcare providers can also explain, in some cases, how a patient may progress over time based on their genetic diagnosis. For example, some types of Alport syndrome are more likely to progress to kidney failure than others. Once a genetic diagnosis is established, one can better understand who else in the family is at risk and may benefit from genetic testing and counseling. If a patient has autosomal dominant polycystic kidney disease, each of their children will have a 50% chance to have the same condition. Reproductive testing options like preimplantation genetic testing or amniocentesis are also available to mitigate or understand the risk for recurrence. Last, but certainly not least, clinical trials are often available for genetic forms of kidney disease. In some cases, one may need genetic testing before being eligible for a clinical trial.
Conclusion
Genetic conditions leading to kidney disease are common in the pediatric population. In many cases, clinical evaluation is not sufficient to accurately diagnose these conditions. Thus, incorporating genetic testing is an important tool for individuals caring for children or adolescents with kidney disease. A genetic diagnosis can impact treatment and medical management for the entire family. For any questions about genetic testing or interpretation, please reach out to a genetics specialist in your area.




